Disc herniations
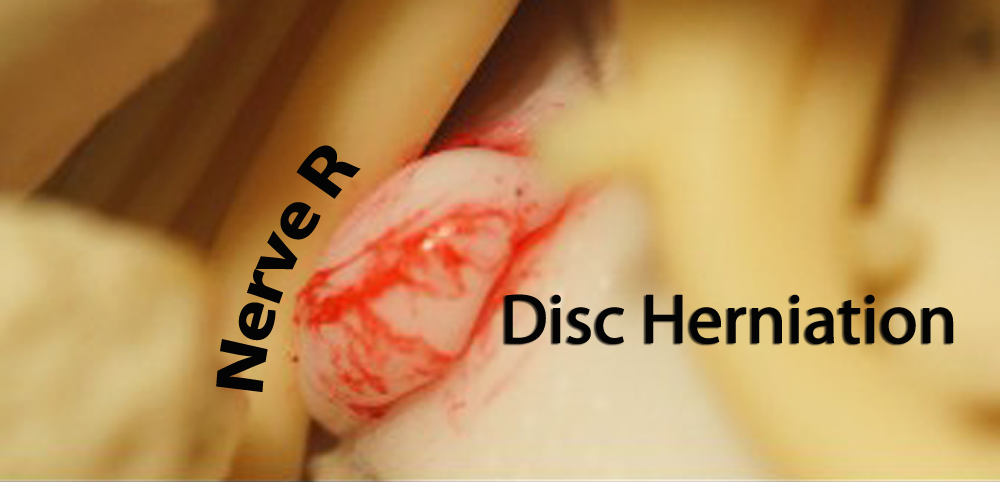
Human spinal column is formed with 33 vertebrae and gelatinous, spongious cartilage structures between them. Nerve roots coming out from medulla spinalis are very close to the intervertebral discs. Sometimes intervertebral discs are damaged and herniated from their natural positions, this may cause nerve root irritations.
This is called “intervertebral disc herniation”, if it is present at the low back region then it is “lumbar disc herniation”. Disc herniations are commonly seen at lumbar levels of vertebra, especially levels called L4-L5 and L5-S1. Mostly pain radiating to the effected level of the leg and/or foot, numbness, tingling and rarely motor deficit may be present.
Bed rest must be the main therapotical modality.
Vertebral MRI is the final and certain diagnosis procedure. Physical examination must be clear to evaluate the pain radiating areas.
Surgery is not the main and certain therapeutical modality for disc herniations. Surgery must be done if severe nerve root compression with motor and/or sensory deficit is present.
Pain therapy interventions are indicated if the herniated disc is not extruded and/or seqestrated from the main body.
Transforaminal injections, intervertebral disc modulations such as nucleoplasty and nucletomy and ozone therapy are some of the interventional techniques for pain relief, debulging of the herniated disc and enforcement for healing of the affected disc and nerve root. Laser nucleotomy is a great alternate for debulging of the disc.
Elderly patients with disc herniations, patients with underlying health conditions such as heart and renal problems are appropriate for interventional pain management techniques for disc herniations.
All of the interventional procedures are outpatient, no general anesthesia is necessary. Patients with anxiety may receive some sedations. All patients are discharged from the hospital few hours after the procedures and they may go back to work in 5-10 days.
info@bigdoctors.com